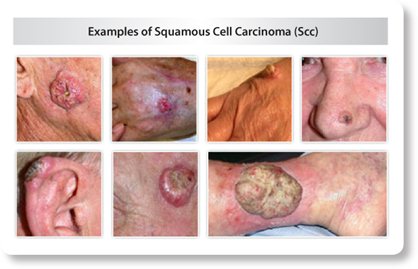
Squamous cell carcinoma (SCC) is the second most common type of skin cancer. If this type of skin cancer is detected early, it can be cured with treatment.
What SCC looks like
SCC can appear in many different forms. It can be a bump that feels crusty and rough, a flat patch that is red and rough, a dome shaped bump that grows and bleeds or a sore that does not heal or that heals and returns.
Most of these types of skin cancer develop on sun exposed skin but they can develop in areas that are not exposed to the sun as well.
Some begin as a precancerous growth called an actinic keratosis (AK). AKs are typically dry, scaly and rough. They can be very small or even as large as a quarter.
Risk factors for SCC
Although SCC can develop on anyone with any skin type, there are certain risk factors that make it more likely for you to develop an SCC at some point in your life. This is more common in caucasians. UV radiation causes damage to the skin and makes it more likely that a skin cancer will develop. As damage accumulates, risk increases. Risk also increases with time because more exposure occurs over time.
The following is a list of risk factors for SCC:
- Pale or light colored skin
- Blue, green or gray eyes
- Blond or red hair
- Inability to tan
- Significant exposure to UV light
- Using tanning beds or sunlamps
- Exposure to cancer causing chemicals
- Smoked or used tobacco
- Spending lots of time near heat, such as a fire
- Previous diagnosis of AKs
- Badly burned skin
- Having an ulcer or sore on the mouth that has been there many years
- Taking medicine that suppresses your immune system
- Receiving an organ transplant
- HPV infection
- Receiving many x-rays
- Many PUVA light treatments
- Medical conditions – Xeroderma Pigmentosum, Epidermolysis Bullous or Albinism
Treatment Options for SCC
Early detection provides the best treatment options for SCC. If it is not treated, it can spread to other areas of the body and make it more difficult to treat.
A biopsy must be performed to get an accurate diagnosis. To have the biopsy performed, numbing medicine is injected into the skin surrounding the possible skin cancer. A sample of tissue is obtained and sent to a pathologist to view under the microscope.
The diagnosis given by the pathologist will determine treatment options. The options available depends on how deep the skin cancer is, how large it is, and whether or not it has spread to other areas.
- Excision – Surgical procedure performed in office. This is performed in the same fashion as the biopsy, with local injections of numbing medicine. The area of skin containing skin cancer, along with normal looking skin is taken off and sent to the pathologist to look at under the microscope. The pathologist will determine if any cancer cells are in the normal looking skin. If there are no cancer cells, then we say that the margins are clear and no further treatment is needed. If there are cancer cells present, more treatment will be needed.
- Mohs Micrographic Surgery – Surgical procedure performed in the office under local anesthesia. This means that injections are given into the skin and you will be awake for the procedure. The surgeon will remove the area of skin that is affected by cancer and a small amount of normal looking skin. He or she will then look at the sample under the microscope immediately to determine whether or not margins are clear. If they are not clear, more skin is taken and the process is repeated until all margins are clear.
- Radiation – When a person cannot undergo surgery to treat a skin cancer, they may be sent for radiation therapy. A series of radiation treatments are used to destroy the cancer cells.
- Medicine applied to the skin – If caught early enough, a prescription medication can be given to be applied to the skin at home to destroy cancer cells.
- Cryotherapy – For superficial SCC, those just on the surface of the skin, liquid nitrogen can be used to destroy cancer cells. A very cold air is applied to the skin, usually by spraying from a canister to “freeze” the cancer cells to destroy them.